Publication dans Science Advances. L’interview de Caroline Arber
« Notre étude apporte un nouvel éclairage sur les programmes génétiques qui transforment les cellules immunitaires en tueurs puissants et durables du cancer » Caroline Arber - médecin associée au Département d’oncologie UNIL CHUV, professeure associée à l’UNIL et membre de la branche lausannoise du Ludwig Institute for Cancer Research - et son équipe ont développé des types spécifiques de cellules immunitaires modifiées qui peuvent servir d'immunothérapie potentielle pour les patients atteints de cancer. Son étude récente montre que les cellules immunitaires conçues comme des cellules hybrides "auxiliaires" et "tueuses" sont les plus puissantes et les plus aptes à améliorer la destruction des tumeurs par rapport aux cellules "tueuses" classiques. Ses travaux ont permis de mieux comprendre les conséquences génétiques de l'ingénierie des cellules immunitaires hybrides et de découvrir des programmes génétiques spécifiques qui peuvent servir de modèle pour développer la prochaine génération d'immunothérapies anticancéreuses basées sur les cellules immunitaires.
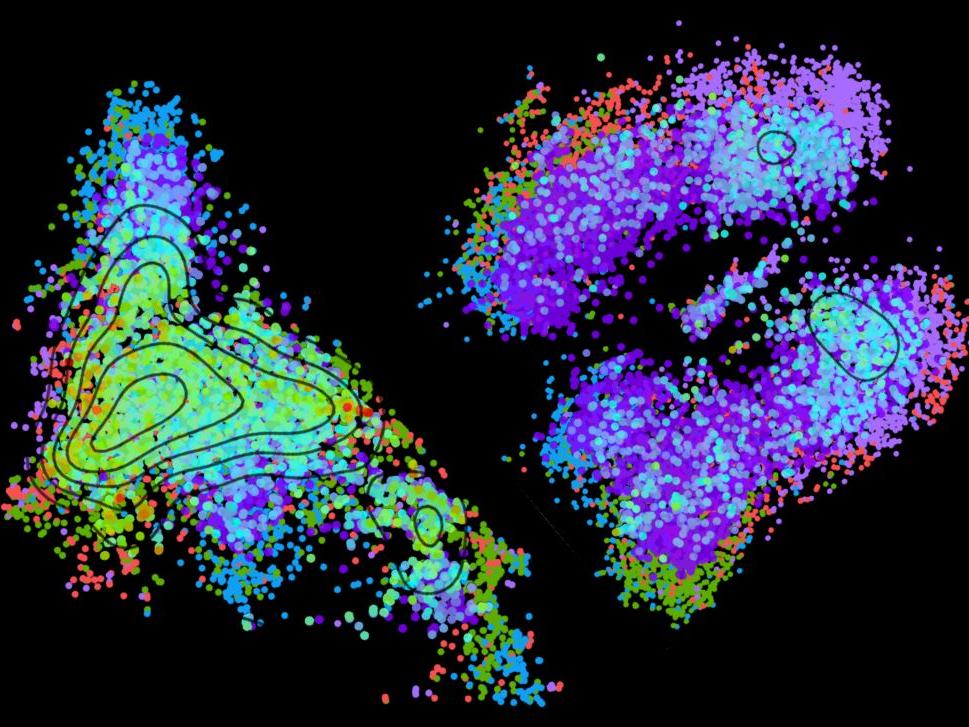
"Our study provides new insight into the genetic programs that turn immune cells into potent and long-lasting killers of cancer”
Caroline Arber and her team have deeply characterized special types of engineered immune cells that can serve as a potential immunotherapy for cancer patients. Her recent study shows that immune cells engineered as hybrid ‘helper’ and ‘killer’ cells are most potent and able to deliver enhanced tumor killing compared to classical ‘killer’ cells. Her work has provided valuable insight into the genetic consequences of engineering hybrid immune cells and uncovered specific genetic programs which can serve as a blueprint for developing next-generation immune cell-based cancer immunotherapies.
What is this paper about?
A specific type of immune cells, called T cells, are part of our defense against foreign elements in our body. Cancer cells are often not sufficiently recognized by our immune system, but technologies allow us to engineer T cells to make them recognize cancer cells much more efficiently. Some of these T cells are able to recognize and kill cancer cells (‘killers’) while others have a more supportive role (‘helpers’). Interestingly, it is possible to make these ‘helper’ T cells become potent cancer killers by genetically modifying them with a protein that is exclusively expressed on ‘killer’ T cells. We were interested in defining which genetic programs could lead to this switch from ‘helper’ to ‘killer’ and used novel gene sequencing technologies to investigate this question. We were surprised to find out that our genetically engineered hybrid ‘helper-killer’ T cells were more efficient in killing cancer cells than the classical ‘killers’. We uncovered multiple genetic programs which are uniquely expressed in our hybrid cells and participate in producing superior function.
How did you decide on this particular avenue of research?
Our lab has a longstanding interest in the development of new T cell-based immunotherapies. Coming from the field of hematopoietic stem cell transplantation that pioneered the concept of cell-based immunotherapy, we are convinced that T cell therapies will be an important cornerstone in the fight against many cancers. We are particularly intrigued by understanding in great detail how our novel therapies work. In this project, we built our strategy upon a protein (called T cell receptor, or TCR) that we have previously identified and that endows ‘killer’ T cells with a high specificity to cancer cells and makes them kill the cancer. Since we know that ‘helper’ T cells play an important role in the long-term control of cancer, we wondered if we can turn ‘helper’ T cells into hybrid cells by introducing the TCR and another molecule that is normally exclusive to ‘killer’ T cells. We extensively interrogated our new hybrid ‘helper-killer’ T cells and compared them to classical ‘killer’ T cells down to the level of single cells. Very little was known so far on the genetic consequences behind this switch from ‘helper’ to ‘killer’ and the hybrid phenotype. Thus, our goal was to unravel the molecular patterns that underlie this reprogramming and make the hybrids more potent killers than the classical killers.
What context does this paper fit into?
The field of cancer immunotherapy is advancing rapidly and allows us to treat cancer patients in a highly personalized way. For certain types of leukemia and lymphoma, efficient commercial cellular therapies are available, but for most cancer patients, this option does not exist yet. Therefore, our priority is to develop and deeply characterize novel engineered T cell therapies with enhanced features compared to the existing ones. Specifically, we aim to develop approaches that target features on cancer cells or in the tumor microenvironment that are not targeted with existing therapies. We aim to engineer T cells with enhanced tumor killing capacity and the capacity to stay alive and function in the body for a long time to keep the cancer under control. Precise understanding of the biology of the enhanced therapies will help us to incorporate this information into the next iteration of T cell therapies.
What and how does it add to that?
Our study is the first to provide solid genetic data at the single cell level underlying the genetic switching of ‘helper’ T cells into hybrid ‘helper-killer’ T cells. We have uncovered multiple genetic programs which can be harnessed for the future development of more efficient immune cell therapies. Our gene sequencing approach has produced a dataset which provides a detailed insight into potential mechanisms that drive the various programs associated with the enhanced function of the engineered hybrid cells.
What is the next step moving on from these findings, for you and your lab?
Our ultimate goal is to develop safe and enhanced T cell-based immunotherapies and move these to the clinic for cancer patients who don’t respond well to existing therapies. The information gained in this study allows us to precisely explore several interesting genes and pathways that we think have the potential to further advance the function of our engineered immune cells. We are also evaluating the possibility to develop a clinical trial with our strategy.
Caroline Arber is a clinician-scientist specialized in hematology and specifically focusing on cell-based immunotherapies for blood cancers. In the clinic at the CHUV she is building the outpatient consultation team in charge of immune effector cell therapies for blood cancers. Her research focuses on developing novel engineered immune effector cell therapies with enhanced features. She is a Médecin Associée at the CHUV Department of oncology UNIL CHUV, an Associate Professor at UNIL, and an Adjunct Scientist at the Ludwig Institute for Cancer Research Lausanne.